
Translation and validation of the Chinese version of Brace Questionnaire (BrQ)
Introduction
Adolescent idiopathic scoliosis (AIS) is the most common form of spinal deformity, with a prevalence of 1% to 2% (1). It has been reported to negatively affect a patient’s health-related quality of life (HRQoL), with complaints of increased back pain, reduced physical activity, and psycho-social problems associated with a disfigured appearance (2,3). Bracing represents the primary form of non-operative management of AIS (4). While most studies suggested its effectiveness, this modality has itself been reported to result in a deterioration of HRQoL among patients who receive bracing treatment (3). Therefore, close monitoring of HRQoL should be performed while under treatment and the impact of bracing on HRQoL should be accounted for in the evaluation of treatment results of AIS patients (5).
Among HRQoL assessment tools dedicated to patients with AIS, the Scoliosis Research Society-22 Questionnaire (SRS-22) is the most widely used (6). However, SRS-22 does not include items specific to the impact of bracing on HRQoL of AIS patients (3). A disease-specific questionnaire (7-9) with proven higher sensitivity than generic patient-oriented counterparts is required (10). To specifically evaluate the HRQoL of AIS patients under bracing treatment, Vasiliadis et al. (11) first introduced the Brace Questionnaire (BrQ), which included eight domains (general health perception, physical functioning, emotional functioning, self-esteem and aesthetics, vitality, school activity, bodily pain and social functioning).
The BrQ was initially developed and validated in Greek, and has been translated into Polish (12), Italian (13), French (14), Korean (15), Turkish (16), and Persian (17) and found to be valid. We herein aimed to culturally adapt and psychometrically validate the contemporary Chinese version of BrQ following the standard protocol of trans-cultural validation as demonstrated in previous literature (18).
Methods
In general, we strictly followed the widely accepted guidelines for translation and cross-cultural adaptation as described by Guillemin (6,18), including independent forward translation, review and reconciliation of differences, reverse translation and establishment of the consensus-based pre-final version by an expert panel.
The pre-final version of Chinese BrQ was presented to 10 Chinese-speaking AIS patients, who were subsequently interviewed on their understanding of each questionnaire item. Each patient was asked to comment on the pre-final version of Chinese-translation of BrQ and to identify any words that they found difficult to understand. Thereafter, their responses were reviewed by the expert panel and the final Chinese version of BrQ was determined by consensus.
We then administered BrQ to 70 consecutive Chinese patients with AIS. Inclusion criteria included age at the time of questionnaire administration between 10 and 18 years, Cobb angle of the primary curve on long-cassette antero-lateral X-ray between 20.0° and 40.0°. All patients were treated with the same kind of brace for at least 4 months and for at least 10 hours per day. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013) and the study was approved by the Ethics Committee of Peking University Third Hospital (No. M2018216) and informed consent was taken from all the patients.
The BrQ comprises of 34 Likert-scale items in eight specific domains: (I) general health perception, (II) physical functioning, (III) emotional functioning, (IV) self-esteem and aesthetics, (V) vitality, (VI) school activity, (VII) bodily pain and (VIII) social functioning. The total score equals the average of each item score multiplied by 20. Item score ranges from 1 to 5 points for each item, with more points indicating higher HRQoL. Therefore, the minimum score of BrQ was 20 and the maximum was 100. Similarly, a sub-scale score can be calculated for each of the eight domains by multiplying the average item score of all items within a certain domain by 20 (11).
The SRS-22 includes five domains (function, pain, mental health, self-image, management satisfaction/dissatisfaction), and a total of 22 items. The item score ranges from 1 to 5 points, and the summary score ranges between 22 and 110 (6). A previously-validated Chinese version of SRS-22 was used in the current study (19,20).
A test-retest design (with a 14-day interval between questionnaire administration) was used to measure the temporal stability of the Chinese version of BrQ using the intra-class correlation coefficient (ICC). The Cronbach’s alpha was used to assess internal consistency. The Pearson’s correlation coefficient was used to evaluate convergent validity by comparing the responses to BrQ against responses to SRS-22. SPSS 26.0 was used for statistical analysis. For all tests, statistical significance was set at P<0.05.
Results
The study took place from February 2019 to January 2020 with the approval of the local hospital ethics committee. A total of 70 consecutive native Chinese-speaking patients with AIS, including 65 girls and 5 boys, were enrolled in this study after obtaining consent from patients and their guardians’ consent, and all of them completed the second survey. The mean patient age was 13.9 [standard deviation (SD), 2.1] years, and the mean Cobb angle was 28.0° (SD, 6.6). Demographics and clinical characteristics were summarized in Table 1.
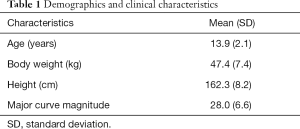
Full table
The questionnaires had no missing values or patient information. Scores from the eight BrQ domains and the five SRS-22 domains were shown in Table 2, respectively, along with their ceiling and floor effects. There were no floor or ceiling effects observed with the total score of BrQ. However, significant ceiling effects were observed in the school activity (45.7%), bodily pain (35.7%), and social functioning (22.9%) domains of BrQ.
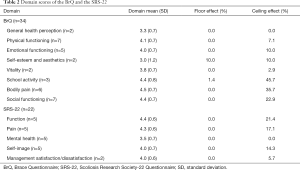
Full table
Excellent test-retest reliability (ICC, 0.967; Table 3) and internal consistency (Cronbach’s alpha, 0.923; Table 4) were demonstrated with the overall BrQ. However, internal consistency was poor in the domain of general health perception (Cronbach’s alpha, 0.399).
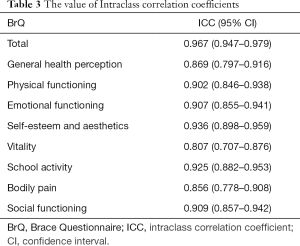
Full table
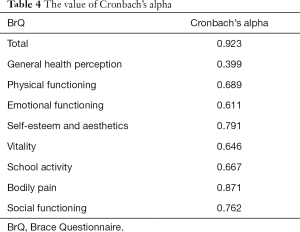
Full table
Statistical analysis
Regarding convergent validity, Pearson’s correlation coefficients varied from very weak to strong across different domains between BrQ and SRS-22 (Table 5). The overall BrQ and SRS-22 scores were strongly correlated with a coefficient of 0.743 (P<0.001).
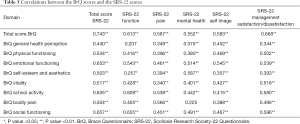
Full table
Discussion
Brace treatment has been used as the primary form of non-operative management of AIS. Many types of brace have been reported in the literature (4). Previous studies suggested that bracing may negatively affect HRQoL of AIS patients (5). On the other hand, declining HRQoL might compromise compliance with bracing and consequently compromise the effectiveness of this treatment modality (3). Therefore, it is important to better evaluate and closely monitor the HRQoL aspects of AIS patients undergoing bracing treatment. SRS-22 has been widely used as an assessment tool for patients with scoliosis (6). However, SRS-22 is not specific to bracing management. In contrast, BrQ was designed specifically for AIS patients wearing braces as their primary treatment modality. Since its publication in 2006, BrQ has undergone cross-cultural adaptation into multiple foreign languages (11-17). Our current study introduced the Chinese version of BrQ following standard protocols of translation and cultural adaptation, which can be used as a clinical evaluation tool for Chinese patients AIS. The culturally adapted Chinese version of BrQ showed good psychometric properties, largely comparable to those of the original Greek version and translated versions in other languages (Table 6).
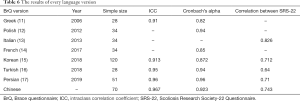
Full table
The optimal inclusion criteria for AIS brace studies include greater than 10 years of age when the brace is first prescribed, Risser sign 0–2, Cobb angle of the primary curve ranges 25–40°, and no prior treatment (4). However, in practice, the Cobb angle of the brace treatment population is wider than this range. Owing to the anxiety of patients and their families’ concerns about the progress of the disease, some patients with a Cobb angle of 10–25 degrees require a brace for treatment. Some patients with a Cobb angle greater than 50 degrees cannot undergo surgical treatment because of their overall physical condition or financial constraints. In the interest of standardization, we only included patients with a Cobb angle between 20 and 40 degrees in our study. For cases of mild scoliosis, previous studies showed that deterioration in HRQoL was not correlated with the Cobb angle (3). One study reported that Cobb angle was not significantly related to the BrQ score (13). Therefore, this study did not use the Cobb angle as a tool for validity evaluation.
In the present study, ceiling effects were observed in 3 domains of BrQ, namely, school activity, bodily pain, and social functioning. Yet the Korean version of BrQ revealed no ceiling effect in any domain (15). This discrepancy was likely due to the fact that Chinese patients stress the importance of adolescent education and seldomly delay going to school.
The test-retest ICC of the Chinese BrQ was 0.967, indicating good temporal stability, similar to previous studies. Moreover, good temporal stability was also shown in each domain. The test-retest interval was 14 days, which was sufficient to eliminate memory effects.
The BrQ total score had a high value of Cronbach’s alpha (0.923), showing high internal consistency similar to other versions. Most domains also showed good internal consistency. However, the general health perception domain failed to exceed the minimum recommended value of 0.40 (a cut-off for acceptable internal consistency). Our results showed that some patients were even more concerned with discomfort associated with brace-wearing (lower score in item 1) than with disease progression (higher score item 2). This might explain the sub-optimal internal consistency of the general health perception domain, in addition to demonstrate how much brace-wearing could negatively affect HRQoL in some patients.
In the analysis of convergent validity, the correlation coefficient between the total score of BrQ and SRS-22 was 0.743 (P<0.001), which showed good convergent validity. Additionally, our data showed that the correlation between the overall as well as individual domain scores of BrQ and different SRS-22 domain scores was all significant but the correlation coefficients varied from very weak to strong. Although items in the BrQ are completely different from those in SRS-22, they share some domains that measure common concepts, such as the physical functioning domain (BrQ) and the function domain (SRS-22), the emotional functioning domain (BrQ) and the mental health domain (SRS-22), the self-esteem and aesthetics domain (BrQ) and the self-image domain (SRS-22), the bodily pain domain (BrQ), and the pain domain (SRS-22). Strong correlation coefficients were observed in domains on the same concept from different instruments, while weak correlation coefficients were observed between domains measuring different concepts.
To conclude, the culturally adapted Chinese version of BrQ showed excellent reliability, high internal consistency, and satisfactory concurrent validity. This instrument is, therefore, useful as a clinical evaluation tool for Chinese patients with AIS. Further research may focus on whether BrQ can supplement SRS-22 or be used as a stand-alone assessment tool in this patient population in the future.
Acknowledgments
Funding: This work was supported by grants from the Young Scientists Fund of the National Natural Science Foundation of China (CN) (No. 2019NSFC81901822), Peking University Fund of Fostering Young Scholars’ Scientific & Technological Innovation (No. BMU2018PYB016) and Capital’s Funds for Health Improvement and Research (No. 2018-4-4097).
Footnote
Data Sharing Statement: Available at http://dx.doi.org/10.21037/tp-20-377
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/tp-20-377). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). The study was approved by the Ethics Committee of Peking University Third Hospital (No. M2018216) and informed consent was taken from all the patients.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Willner S, Uden A. A prospective prevalence study of scoliosis in Southern Sweden. Acta Orthop Scand 1982;53:233-7. [Crossref] [PubMed]
- Danielsson AJ, Wiklund I, Pehrsson K, et al. Health-related quality of life in patients with adolescent idiopathic scoliosis: a matched follow-up at least 20 years after treatment with brace or surgery. Eur Spine J 2001;10:278-88. [Crossref] [PubMed]
- Tones M, Moss N, Polly DW Jr. A review of quality of life and psychosocial issues in scoliosis. Spine (Phila Pa 1976) 2006;31:3027-38. [Crossref] [PubMed]
- Richards BS, Bernstein RM, D'Amato CR, et al. Standardization of criteria for adolescent idiopathic scoliosis brace studies: SRS Committee on Bracing and Nonoperative Management. Spine (Phila Pa 1976) 2005;30:2068-75; discussion 2076-7. [Crossref] [PubMed]
- Aulisa AG, Guzzanti V, Perisano C, et al. Determination of quality of life in adolescents with idiopathic scoliosis subjected to conservative treatment. Scoliosis 2010;5:21. [Crossref] [PubMed]
- Asher M, Min Lai S, Burton D, et al. The reliability and concurrent validity of the scoliosis research society-22 patient questionnaire for idiopathic scoliosis. Spine (Phila Pa 1976) 2003;28:63-9. [Crossref] [PubMed]
- Aprile I, Ruggeri AE, Savi Scarponi F, et al. Health-related quality of life in patients with adolescent idiopathic scoliosis after treatment: short-term effects after brace or surgical treatment, a comment. Eur Spine J 2007;16:1962-3; author reply 4. [Crossref] [PubMed]
- Padua R, Ceccarelli E, Aulisa AG, et al. Outcome of Harrington surgery for idiopathic scoliosis. SF-36 and Roland questionnaires assessment. Stud Health Technol Inform 2002;88:404. [PubMed]
- Padua R, Padua S, Aulisa L, et al. Patient outcomes after Harrington instrumentation for idiopathic scoliosis: a 15- to 28-year evaluation. Spine (Phila Pa 1976) 2001;26:1268-73. [Crossref] [PubMed]
- Guyatt GH, Bombardier C, Tugwell PX. Measuring disease-specific quality of life in clinical trials. CMAJ 1986;134:889-95. [PubMed]
- Vasiliadis E, Grivas TB, Gkoltsiou K. Development and preliminary validation of Brace Questionnaire (BrQ): a new instrument for measuring quality of life of brace treated scoliotics. Scoliosis 2006;1:7. [Crossref] [PubMed]
- Kinel E, Kotwicki T, Podolska A, et al. Polish validation of Brace Questionnaire. Eur Spine J 2012;21:1603-8. [Crossref] [PubMed]
- Aulisa AG, Guzzanti V, Galli M, et al. Validation of Italian version of Brace Questionnaire (BrQ). Scoliosis 2013;8:13. [Crossref] [PubMed]
- Deceuninck J, Tirat-Herbert A, Rodriguez Martinez N, et al. French validation of the Brace Questionnaire (BrQ). Scoliosis Spinal Disord 2017;12:18. [Crossref] [PubMed]
- Lim JM, Goh TS, Shin JK, et al. Validation of the Korean version of the Brace Questionnaire. Br J Neurosurg 2018;32:678-81. [Crossref] [PubMed]
- Gür G, Yakut Y, Grivas T. The Turkish version of the Brace Questionnaire in brace-treated adolescents with idiopathic scoliosis. Prosthet Orthot Int 2018;42:129-35. [Crossref] [PubMed]
- Rezaee S, Jalali M, Babaee T, et al. Reliability and Concurrent Validity of a Culturally Adapted Persian Version of the Brace Questionnaire in Adolescents With Idiopathic Scoliosis. Spine Deform 2019;7:553-8. [Crossref] [PubMed]
- Guillemin F. Cross-cultural adaptation and validation of health status measures. Scand J Rheumatol 1995;24:61-3. [Crossref] [PubMed]
- Li M, Wang CF, Gu SX, et al. Adapted simplified Chinese (mainland) version of Scoliosis Research Society-22 questionnaire. Spine (Phila Pa 1976) 2009;34:1321-4. [Crossref] [PubMed]
- Qiu G, Qiu Y, Zhu Z, et al. Re-evaluation of reliability and validity of simplified Chinese version of SRS-22 patient questionnaire: a multicenter study of 333 cases. Spine (Phila Pa 1976) 2011;36:E545-50. [Crossref] [PubMed]


