
Autism spectrum disorder: psychological and functional assessment, and behavioral treatment approaches
Introduction
Autism, first described in 1943 by Leo Kanner, was at that time thought to be a rare disorder (1). In the past two decades, the prevalence of Autism has seen a consistent and dramatic increase with the diagnostic criteria changing to encompass a broader perspective of symptom manifestations, now called autism spectrum disorders (ASD), which has led to increased knowledge and push for earlier screening and recognition of the disorder. In the past, the ASD were historically made up of multiple distinct disorders (i.e., autistic disorder, pervasive developmental disorder—not otherwise specified and Asperger disorder). In 2013, the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), these disorders were combined into one term Autism Spectrum Disorder. The most recent estimate from the Centers for Disease Control and Prevention (CDC) is that 1 in 68 children has a diagnosis of ASD (2). In 2016, The American Academy of Pediatrics recommended all children be screened for ASD at ages 18 and 24 months and for all children who fail routine developmental surveillance. Many studies have been published on emerging theories for the pathophysiology and etiology of ASD, most concluding the cause is multi-factorial with a complex interplay of several mechanisms, genetics, epigenetics, and environmental factors (1). The disorder represents a heterogeneous set of neurodevelopmental disorders with a typical triad of symptoms, which includes problems with social interaction, language, and communication abnormalities and stereotypical behavior, characterized as ritualistic, repetitive, and restrictive behaviors (2).
Given the variation in children’s manifestations of ASD, degrees of co-morbid conditions as well as differences in level of functioning for children illustrate the need for a clear understanding of the diagnostic categories as well as the variety and purpose of each screening test. Further, the understanding of the recommendations for treatment are of vital importance for practitioners. This manuscript should be a valuable resource guide for health practitioners
Autism assessment
Primary care screening tools (MCHAT and MCHAT follow-up)
Screening tools are not used to establish a diagnosis, but rather to aid in identifying those that might need further evaluation. If a child fails on a screening test, they will be referred to a specialist to receive a comprehensive clinical evaluation to determine a potential diagnosis. The AAP currently recommends routine developmental screening at ages 9-, 18-, 24-, and 30-month well-child visits. During these visits, the pediatrician ensures normal developmental marks are reached.
There is debate as to whether specific screening for ASD, when no parental concerns have been raised, should be universal. In addition to this routine screening, the AAP recommends that screening specifically for autism also be performed at ages 18–24 months in all children, with the rationale that earlier intervention is associated with better outcomes. Studies suggest that intervention before 3 years of age has the greatest impact (3). Additionally, studies have shown that screening leads to earlier referral and diagnosis (4). The U.S. Preventive Services Task Force 2016 recommendation, however, stated that there is not enough evidence to assess the benefits and harms of screening ASD in asymptomatic children in the 18–30 months age range, and called for more research (5). Those that argue against universal screening are wary of the false positives, and the unnecessary referrals and misuse of resources that would result (6). While screening tests are aimed at identifying autism before 24 months, the median age of diagnosis in the US is approximately 4.5 years old (7).
Screening tools can be classified as either level 1 or level 2. The purpose of level 1 screening is to identify children at risk for an ASD and is thereby intended to be used on all children. Level 2 screening, on the other hand, is administered by a diagnostic clinic to a referred population, and meant to differentiate between children at risk for an ASD and other developmental disorders (8). There are various tools for both levels of screening. Here we mention a few of those most utilized.
Level 1 screening tools
Various screening tools have been developed with the goal of achieving optimal sensitivity and specificity. A recent meta-analysis of the accuracy of level 1 screening tests had a pooled sensitivity of 0.72 and a pooled specificity of 0.98, and concluded that these tools show statistically significant results and are adequate to detect autism in the 14–26 months range (9).
MCHAT and the MCHAT revised/follow-up
The Checklist for Autism in Toddlers (CHAT) was the first screening tool, but was revised to the MCHAT in 1999 to improve sensitivity. The MCHAT-revised followed in 2009 (10). The MCHAT-R/F includes a follow-up questionnaire for those that screen positive, with the purpose of reducing the number of false positives. The M-CHAT is the most well used screening tool in the US and in Europe. It is indicated for children in the 18–24 months range.
The Q-CHAT
The Q-CHAT is an extended version of the CHAT. It covers a broader range of ASD symptoms, which are rated on a 5-point scale (rather than present/absent).
The Social Communication Questionnaire (SCQ)
The SCQ offers a screening instrument for ASD validated for children age 4 years or older. It consists of a 40-item, parent-reported screening measure. While it is a screening tool, it is based on the Autism diagnostic interview, which is a parent interview conducted by a clinician as the next step in diagnosis (11).
The Infant Toddler Checklist (ITC)
The ITC is a sub-part of the Communication and Symbolic Behavior Scales, a tool used to identify non-autism specific communication abilities of children between 6 months and 2 years. The ITC identifies children between the ages of 6 to 24 months of age who have any type of communication delay, including ASD (12).
First Year Inventory (FYI)
The FYI is 62-item caregiver-rated tool indicated for 12-month-old shown to have modest sensitivity. This tool is still under development (12).
Level 2 screening tools
The Screening Tool for Autism in Toddles and Young Children (STAT)
The STAT is a screening tool designed for children when developmental concerns are suspected, between 24 and 36 months of age. It consists of 12 activities assessing play, communication, and imitation skills. It requires a higher level of expertise to administer than the M-CHAT, as it is based on specific interactions (12).
The Systematic Observation for Red Flags (SORF)
The SORF is an observational screening measure for 16–24-month-old who have received the Communication and Symbolic Behavior Scales. It may be better at detecting children with higher developmental scores (13).
The Autism Observation Scale for Infants (AOSI)
The AOSI
Intellectual assessments (Table 1)

Full table
Wechsler Adult Intelligence Scale-IV (WAIS-IV)
The WAIS-IV Is used to measure intelligence and cognitive ability in adults and older adolescents. The assessment has undergone several revisions and is currently undergoing under revision slated to be released sometime in 2021. The WAIS is the most widely used intellectual assessment around the world. The current version is composed of 10 core subtests as well as five supplemental subtests. The full-scale IQ is derived from the combination of the 10 core subtests (15).
The assessment is separated into four main index scores that ultimately represent what is understood to be the components of intelligence. These index scores include a Verbal Comprehension Index, Perceptual Reasoning Index, Working Memory Index, and a Processing Speed Index.
The tasks included in the Verbal Comprehension Index measure abstract verbal reasoning, semantic knowledge, verbal comprehension and expression, degree of general information acquired from culture, and the ability to express abstract social conventions, rules and expressions. The Perceptual Reasoning Index measures visual spatial processing, problem solving, visual motor construction, nonverbal abstract problem solving, inductive reasoning, visual spatial reasoning, and quantitative reasoning. The Working Memory Index includes tasks that measure attention, encoding, auditory processing, quantitative reasoning, concentration, and mental manipulation of numbers. The Processing Speed Index includes tasks related to how quickly an individual can complete a task of coding and target symbols, associative memory, and graphomotor speed (16).
Wechsler Intelligence Scale for Children (WISC)-V
The WISC is used to measure a child’s general intellectual ability. It provides five main indices that include Verbal Comprehension, Visual Spatial, Fluid Reasoning, Working Memory, and Processing Speed. The assessment helps determine if a child has any specific learning disabilities as well. The WISC is comparable to the WAIS-IV in measuring similar indices.
Mullen scales of early learning
The Mullen is used as a developmental measure of cognitive development. The assessment is broken down into five main scales including visual reception, gross motor, fine motor, receptive language, and expressive language. The Mullen generates a score at the end that is used as an estimate of overall intelligence (17).
Universal Test of Nonverbal Intelligence (UNIT)
The UNIT is an assessment used as an alternative to traditional intellectual assessments. It is used to provide an assessment of nonverbal intelligence. The assessment is made up of six main subtests including symbolic memory, spatial memory, object memory, cube design, analogic reasoning, and mazes.
The Symbolic Memory subtest measures short-term visual memory and complex sequential memory. The Spatial Memory subtest measures short-term visual memory. The Object Memory subtest measures short-term recognition and recall of significant symbolic material. The Cube Design subtest measures visual-spatial reasoning. The Analogic Reasoning subtest measures symbolic reasoning. The Maze subtest measures reasoning and planning skills.
The UNIT is further organized into four scales: memory, symbolic, reasoning, and non-symbolic. The combination of these scores accumulates to the Full-Scale Intelligence Quotient. The Memory Quotient measures complex memory functioning such as short-term recall and recognition of common and conceptualization. The Symbolic Quotient measures problem solving. The Reasoning Quotient measures thinking and problem-solving skills in known and unknown situations and problems. The Non-symbolic Quotient measures problem solving skills with conceptually ambiguous and non-meaningful information (18).
Vineland adaptive scales
The Vineland instrument is a valid and reliable tool used in child and adolescent populations to assess individuals with intellectual disabilities, developmental disorders, and other delays. The tool has three main domains including: socialization, communication, and daily living and correspond to the three domains of adaptive functioning (social, conceptual, and practical) (19). Clinicians typically use this tool for diagnostic purposes or for treatment planning. Additionally, it is used to examine the type and amount of special assistance an individual with a disability may need. Special assistance can include services such as in-home support, special education and vocational training, and assistance with living arrangements such as group homes or personal care attendants.
Speech & language assessment
The presence of a language delay or impairment is one of the primary diagnostic criteria for diagnosis of ASD. Children are being diagnosed earlier with ASD and language skills are heterogenous and an important predictor of later outcome. Several diagnostic screening tests for speech and language exist and can help to define different aspects of abilities for expressive and receptive language. It is important to distinguish between language and speech delay from other causes and ASD. It is important to characterize the strengths and weaknesses of language abilities in children with ASD to plan which treatment plan would work best as well as helping to further define which phenotype the child has for ASD. There are several tests that are utilized to characterize different aspects of speech and language acquisition and skills which help to define the problem area for the specific patient. The tests are as follows.
Peabody Picture Vocabulary Test–V (PPVT-V)
This is an untimed test of receptive vocabulary for Standard American English and is intended to provide a quick estimate of the examinee’s receptive vocabulary ability. It is one of the more commonly used assessment tests for measuring verbal ability. It can be used from ages 2 to 90 years of age. The test has multiple uses such as determining scholastic ability, revealing high and low verbal abilities and helps to determine possible learning disabilities. It can be used to identify language disorders for children with delayed emotional and mental development to assess their verbal intelligence which is helpful in ASD. It is a short test lasting 20–30 minutes.
Clinical Evaluation of Language Fundamentals (CELF-5)
This test is designed to assess a student’s language and communication skills in a variety of contexts, to determine the presence of a language disorder, and describe the nature of the language disorder and plan for treatment. The newest version allows the clinicians to evaluate a student’s general language ability and obtain information that will assist in determining if the student has a language disorder by administering four to six tests. Once it is determined that the student has a language disorder, the assessment process can extend to identifying significant differences in comprehension and expression. The test determines weaknesses of students in the area of morphology and syntax or semantics, as well as how the oral language disorder affects the student’s written language skills, and social language interactions which are key for ASD patients. The test is flexible which allows one to administer only the tests needed to correspond to the objectives for assessment and evaluation This information is an important part of the total assessment process that can be used to collect evidence about a student’s communication abilities in multiple contexts. The CLEF-5 has a better balance of items across receptive and expressive modalities and language content and structure than the previous versions. It maintains standardized test scores and composite scores as well as growth scale values to help measure a student’s progress over time.
Expressive Vocabulary Test–third edition
It is an individually administered norm-referenced instrument that assesses expressive vocabulary and word retrieval for children and adults. The test is useful to supplement quantitative information provided by standard scores and may assist in developing hypotheses about an individual’s test performance and vocabulary abilities.
Pre-school Language Scale–fifth edition
This test is designed to assess receptive and expressive language abilities in children aged 0- to determine the presence of a language delay or disorder. The test consists of an auditory comprehension scale and expressive communication scale to evaluate specific areas of strength and weakness. The test particularly focuses on identifying receptive and expressive language skills in the areas of attention, gesture, play, vocal development, social communication, vocabulary concepts, language structure, integrative language, and emergent literacy. The test aids the clinician in determining the presence and type of language disorder (receptive, expressive, and mixed), eligibility for services and to design interventions based on norm-referenced criterion scores.
The importance of characterizing the relative strengths and weaknesses in the language abilities of individuals with ASD is helpful for planning effective interventions and helps further define which neurocognitive phenotype is associated with ASD (20). The different profiles of language impairment defined with testing helps to discriminate among subgroups of children with ASD, which can lead to further identification of the psychological factors and cognitive mechanisms underlying ASD phenotypes (21).
Autism specific assessments (Table 2)
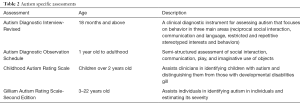
Full table
Autism Diagnosis Interview-Revised (22)
The Autism Diagnostic Interview-Revised is an assessment given between the parents of the individual and the assessor in the form of an interview. The interview includes questions about social interactions, communication, language, and behavior patterns. The questions consist of past and current behaviors as well as the quality of interactions throughout the individual’s development. The assessor will go through nearly one-hundred questions that consist of information about repetitive and restricted behavior, responding to others, smiling, greetings, emotions, comforting, and several other areas. This information is then scored and combined to give a rating and combined with other assessment information to give a diagnosis.
Autism Diagnostic Observation Schedule (ADOS) (23)
The ADOS is an assessment used for autism. The ADOS consists of structured and semi-structured subtests that involve different components of social interactions and communication. The assessment has five modules. The module is chosen based on the individual’s developmental level. The first module is used with children who use few or no speech. Clients who use phrases in their speech but do not speak fluently go through the second module. Module three is for younger individuals who speak fluently while the fourth module is used for adolescents and adults whom are verbally fluent. The fifth module is used for toddlers (24).
Childhood Autism Rating Scale (CARS)
The CARS is used by clinicians to help determine the children who meet criteria for ASD from those who meet criteria for other developmental delays. The scale is a fifteen-item questionnaire that asks about relationships, imitative behavior, emotional responses, ability to adapt to change, use of the senses and sensitivity to foods, sounds, objects, intellectual response, verbal communication, and activity level (25).
Gilliam Autism Rating Scale (GARS)–second edition (26)
The GARS assists clinicians in identifying the severity of autism in individuals whom are 3–22 years old. The scale queries on several dimensions include the stereotypical and characteristic behavior of those with autism, social interactions, and communication skill (27).
Diagnosis
The criteria for ASD includes deficits in social communication, social interaction (across multiple contexts), restricted and repetitive patterns of behavior (lining up toys, rigid thinking patterns, preoccupation with unusual objects, adverse response to specific sounds, interests, or activities that occur in early development and must impair social, occupational, or other important areas of functioning. Additionally, these deficits must not be explained by intellectual disability or developmental delays. Further, ASD can have specifiers such as with or without intellectual or language impairments, association with a medical or genetic condition, or catatonia (28).
History of treatment
The current use of the DSM-5 category for ASD encompasses two domains of function; deficits in social communication and the presence of restricted interests and repetitive behaviors, and allows for broader inclusion of symptoms for diagnosis, and made use of specifiers important to characterize individual patient profiles as well as indication of severity. Treatment for ASD is individualized based on the patient’s needs and involves a multi-disciplinary approach, with primary care medical home and coordination with intensive behavioral therapy, educational programming and ancillary services such as speech/language, occupational and physical therapy services. Depending on the patient’s profile, and severity as well as existence of any co-morbid conditions, treatment includes use of psychopharmacologic medications to target specific symptoms. Patients with ASD may also have co-morbid diseases such as epilepsy, metabolic abnormalities, sleep disturbances or ADHD. Treatment includes medication as needed for those conditions.
Behavioral and education therapies are the mainstay of treatment for ASD. Children younger than 3 years of age should be assessed by an early intervention team and an individualized family service plan should be developed, which includes referral for both developmental and autism-intensive services. Children older than age 3 years of age should be referred to their local public school for school evaluation and determination of the special education eligibility and services needed (29).
Early intensive behavioral interventions as the mainstay for treatment has been shown to help young children with ASD gain skills and improve long-term outcomes (30). The gold standard treatment is Applied Behavior Analysis (30).
Behavioral treatment approaches
Applied Behavioral Analysis (ABA)
ABA therapy has repeatedly demonstrated improvements in cognitive, language, adaptive, and social impairments in children with ASD (31,32). There are many variations on ABA therapy, but all share similar principles. The theory of ABA, stemming from the research of B.F Skinner, is based on the principle that behaviors are shaped through consequences, such as praise or reward. Behaviors that are followed by a reward should increase in frequency, and those that are not will decrease over time (33).
ABA therapy commonly uses discrete-trial teaching (DTT), a technique where skills are taught in a repeated, structured manner. In DTT, the provider collects data on the child’s correct and incorrect answers and then uses this information to determine whether goals are met and adjusts therapy appropriately. Early Intensive Behavioral Intervention is a term for an ABA program with intensive one-one-one direct-trial teaching of up to 40 hours per week (31).
Alternatives to ABA
One criticism of traditional ABA therapy is it increases an individual’s exposure to failed attempts on the repetitive trials, which might decrease motivation. Additionally, the highly structured discrete trial may limit generalizability of learned behaviors (34). There are several variations on ABA therapy that were developed with the goal of naturally inducing desirable behaviors in the child’s own play environment.
Naturalistic Developmental Behavioral Intervention (NDBI)
NDBI is a variation on ABA therapy, also referred to as the Developmental Social Pragmatic model (DSP) (35). The emphasis is on the teaching that occurs in the child’s natural learning environments, and weaving interventions into the child’s own routine. The goal is oriented towards the child’s spontaneous response rather than a cued response elicited during a structured format. NDBI has shown promising effects on improving specifically social engagement and cognition (36). Some therapies combine both ABA and DSP.
Pivotal Response Training (PRT)
PRT utilizes concepts from ABA. In contrast to ABA therapy however, it reinforces both correct responses and any valid attempts made by the child, with the intention of increasing exposure to positive reinforcement and increasing motivation. It is a play-based method that targets “pivotal” developmental areas (motivation, initiation, self-regulation, and response to multiple cues) rather than individual behaviors, with the idea that by targeting these areas, improvements in other areas will follow (37).
Social Skills Therapy
Children with ASD may need help in learning how to act in different types of social situations. Children with ASD often desire for more peer interaction, however, when integrated with their peers they may be at increased risk for peer rejection and social isolation.
Social skills therapy is often taught in a group session that combines direct instruction with an opportunity to practice and generalize these skills. Some evidence shows that social skills groups can improve social competence for children and adolescents with ASD (37). However, most studies on social skills therapy are only on participants who are considered “high functioning” and/or with IQ scores >70, therefore more research is needed.
Ancillary treatments
Speech
Children with ASD may have various impairments in speech and language development. The lack of joint-attention and social skills development likely contribute to an abnormal language development. Speech therapy can be used to improve spoken language as well as initiate learning of nonverbal skills such as gestures. In what is termed Alternative Augmentative Communication (AAC), sign language, pictures (Picture Exchange Communication system), and technology such as iPads can be used as speech tools. Visual-graphic systems allow the individual to rely on recognition rather than recall memory to comprehend language (38).
Occupational therapy
The restrictive or repetitive interests and behaviors of people with ASD may be related to difficulty in processing and integrating sensory information (39). Individuals with ASD are often described as picky or selective eaters. It is suggested that this is due to atypical oral sensory processing (40).
Occupational therapy is currently the mainstay of treatment for sensory disorders associated with ASD. The occupational therapist assesses how the patient’s sensory profile is impacting their ability to complete daily activities and routines.
Physical therapy
Those with ASD demonstrate atypical motor development and delay in motor milestones achievements. Specifically, hypotonia, motor apraxia, toe walking, and gross motor delays may be present (41,42). Physical therapy can help address these motor deficits by improving strength, coordination, and balance.
Other therapies
In some studies, massage therapy improved sensory challenges and ASD symptoms. However more quality studies without the risk of bias are needed. Other sensory therapies such as music therapy and Auditory Integration therapy has limited evidence for positive effects (43).
Additionally, Equine therapy may improve irritability and hyperactivity in children with secondary outcomes of improved social communication and new word acquisition (44). Hyperbaric oxygen therapy has yet to show a proven benefit (45). Children with ASD have higher rates of comorbidities than in typically developing youth or youth with other behavioral conditions. Cognitive Behavioral therapy may be beneficial in treating anxiety as well as a few core autism symptoms (Danial & Wood, 2013).
Conclusions
There have been significant updates to the diagnosis of Autism over time. The evolution of the disorder and the criteria have evolved to appear on a spectrum of severity rather than separate disorders. Within the time of these changes, there have been several screening and assessment tools developed to assist clinicians in correctly diagnosing individuals. Further, assessment tools have now included screeners that can be used in the primary care setting that can be administered by physicians or psychologists who work as an integrated behavioral health team. The screeners used in the primary care setting are particularly helpful to physicians because they save the physician time and the psychologists or the physician can view the screener and assist with appropriate referrals and resources. These updated tools have helped to decrease the misdiagnosis of Autism and have helped lead those with Autism to the services they need. Additionally, through the evolution of Autism, several therapies and interventions have been created to help improve the quality of life of individuals who have the associated deficits. Although several successful interventions exist, research is still needed on other less used and less known or newer approaches music therapy, auditory integration therapy, equine therapy, and hyperbaric oxygen therapy.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Mukherjee SB. Autism Spectrum Disorders- Diagnosis and Management. Indian J Pediatr 2017;84:307-14. [Crossref] [PubMed]
- Yenkoyan K, Grigoryanb A, Fereshetyana K, et al. Advances in understanding the pathophysiology of autism spectrum disorders. Behav Brain Res 2017;331:92-101. [Crossref] [PubMed]
- Sturner R, Howard B, Bergmann P, et al. Autism Screening With Online Decision Support by Primary Care Pediatricians Aided by M-CHAT/F. Pediatrics 2016;138:3. [Crossref] [PubMed]
- Miller JS, Gabrielsen T, Villalobos M, et al. The Each Child Study: Systematic Screening for Autism Spectrum Disorders in a Pediatric Setting. Pediatrics 2011;127:866-71. [Crossref] [PubMed]
- Siu AL. Screening for autism spectrum disorder in young children US preventive services task force recommendation statement. JAMA 2016;315:691-6. [Crossref] [PubMed]
- Sheldrick RC, Garfinkel D. Is a Positive Developmental-Behavioral Screening Score Sufficient to Justify Referral? A Review of Evidence and Theory. Acad Pediatr 2017;17:464-70. [Crossref] [PubMed]
- Baio J, Wiggins L, Christensen DL, et al. Prevalence of Autism Spectrum Disorder Among Children Aged 8 Years — Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2014. MMWR Surveill Summ 2018;67:1-23. [Crossref] [PubMed]
- Soares NS, Patel DR. Office screening and early identification of children with autism. Pediatr Clin North Am 2012;59:89-102. [Crossref] [PubMed]
- Sánchez-García AB, Galindo-Villardón P, Nieto-Librero AB, et al. Toddler Screening for Autism Spectrum Disorder: A Meta-Analysis of Diagnostic Accuracy. J Autism Dev Disord 2019;49:1837-52. [Crossref] [PubMed]
- Robins DL. Screening for autism spectrum disorders in primary care settings. Autism 2008;12:537-56. [Crossref] [PubMed]
- Marvin AR, Marvin DJ, Lipkin PH, et al. Analysis of Social Communication Questionnaire (SCQ) Screening for Children Less Than Age 4. Curr Dev Disord Rep 2017;4:137-44. [Crossref] [PubMed]
- Zwaigenbaum L, Bauman ML, Fein D, et al. Early Screening of Autism Spectrum Disorder: Recommendations for Practice and Research. Pediatrics 2015;136:S41-59. [Crossref] [PubMed]
- Dow D, Guthrie W, Stronach ST, et al. Psychometric analysis of the Systematic Observation of Red Flags for autism spectrum disorder in toddlers. Autism 2017;21:301-9. [Crossref] [PubMed]
- Bryson SE, Zwaigenbaum L, McDermott C, et al. The autism observation scale for infants: Scale development and reliability data. J Autism Dev Disord 2008;38:731-8. [Crossref] [PubMed]
- Lichtenberger EO, Kaufman AS. Essentials of WAIS-IV Assessment (Essentials of Psychological Assessment). 2nd edition. Hoboken, New Jersey: John Wiley & Sons, 2013.
- Benson N, Hulac D, Kranzler J. Independent Examination of the Wechsler Adult Intelligence Scale—Fourth Edition (WAIS–IV): What Does the WAIS–IV Measure? Psychol Assess 2010;22:121-30. [Crossref] [PubMed]
- Staples KL, MacDonald M, Zimmer C. Assessment of motor behavior among children and adolescents with autism spectrum disorder. Int Rev Res in Dev Disabil 2012;42:179-214. [Crossref]
- Nelson BR, Morillas-Brown A, Boyd G. Universal Nonverbal Intelligence Test. In: Goldstein S, Naglieri JA. editors. Encyclopedia of Child Behavior and Development. Boston, MA: Springer, 2011.
- Becker-Weidman A. Effects of early maltreatment on development: a descriptive study using the Vineland Adaptive Behavior Scales-II. Child Welfare 2009;88:137-61. [PubMed]
- Charman T, Jones R, Pickles A, et al. Defining the Cognitive Phenotype of Autism. Brain Res 2011;1380:10-21. [Crossref] [PubMed]
- Tager-Flusberg H, Joseph RM. Identifying neurocognitive phenotypes in autism. Philos Trans R Soc Lond B Biol Sci 2003;358:303-14. [Crossref] [PubMed]
- Tadevosyan-Leyfer O, Dowd M, Mankoski R, et al. A principal components analysis of the Autism Diagnostic Interview-Revised. J Am Acad Child Adolesc Psychiatry 2003;42:864-72. [Crossref] [PubMed]
- Lord C, Risi S, Lambrecht L, et al. The Autism Diagnostic Observation Schedule–Generic: a standard measure of social and communication deficits associated with the spectrum of autism. J Autism Dev Disord 2000;30:205-23. [Crossref] [PubMed]
- Lord C, Rutter M, Good S, et al. Autism diagnostic observation schedule: a standard observation of communicative and social behavior. J Autism Dev Disord 1989;19:185-212. [Crossref] [PubMed]
- Ozonoff S, Boodlin-Jones B, Solomon M. Evidence-based assessment of autism spectrum disorder in children and adolescents. J Clin Child Adolesc Psychol 2005;34:523-40. [Crossref] [PubMed]
- Hutchins T, editor. Gilliam JE. Gilliam Autism Rating Scale – Second Edition (GARS-2). Test review of the Gilliam autism rating scale- third edition. The twentieth mental measurements yearbook; 2017.
- Garro A. Review of the Gilliam autism rating scale-second edition. Seventeenth mental measurements yearbook with tests in print. Buros Institute of Mental Measurement. Lincoln: University of Nebraska Press, 2006.
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th edition. Arlington, VA: American Psychiatric Association; 2013.
- Baumer N, Spence SJ. Evaluation and Management of the Child with Autism Spectrum Disorder. Continuum (MINNEAP MINN) 2018;24:248-75. [Crossref] [PubMed]
- Lock J, La Via MC. Practice Parameter for the Assessment and Treatment of Children and Adolescents with Eating Disorders. J Am Acad Child Adolesc Psychiatry 2015;54:412-25. [Crossref] [PubMed]
- Weitlauf AS, McPheeters ML, Peters B, et al. Therapies for Children With Autism Spectrum Disorder: Behavioral Interventions Update. Rockville (MD): Agency for Healthcare Research and Quality (US), 2014.
- Roane HS, Fisher W, Carr JE. Applied Behavior Analysis as Treatment for Autism Spectrum Disorder. J Pediatr 2016;175:27-32. [Crossref] [PubMed]
- Lei J, Ventola P. Pivotal response treatment for autism spectrum disorder: current perspectives. Neuropsychiatr Dis Treat 2017;13:1613-26. [Crossref] [PubMed]
- Smith T, Iadarola S. Evidence Base Update for Autism Spectrum Disorder. J Clin Child Adolesc Psychol 2015;44:897-922. [Crossref] [PubMed]
- Tiede G, Walton KM. Meta-analysis of naturalistic developmental behavioral interventions for young children with autism spectrum disorder. Autism 2019;23:2080-95. [Crossref] [PubMed]
- Reichow B, Steiner AM, Volkmar F. Cochrane review: social skills groups for people aged 6 to 21 with autism spectrum disorders (ASD). Evid Based Child Health 2013;8:266-315. [Crossref] [PubMed]
- Nunes DRP. AAC interventions for autism: A research summary. Int J Spec Educ 2008;23:17-26.
- Hazen EP, Stornelli JL, O'Rourke JA, et al. Sensory symptoms in autism spectrum disorders. Harv Rev Psychiatry 2014;22:112-24. [Crossref] [PubMed]
- Chistol LT, Bandini LG, Must A. Sensory Sensitivity and Food Selectivity in Children with Autism Spectrum Disorder. J Autism Dev Disord 2018;48:583-91. [Crossref] [PubMed]
- Fournier KA, Hass CJ, Naik SK, et al. Motor coordination in autism spectrum disorders: A synthesis and meta-analysis. J Autism Dev Disord 2010;40:1227-40. [Crossref] [PubMed]
- Ming X, Brimacombe M, Wagner GC. Prevalence of motor impairment in autism spectrum disorders. Brain Dev 2007;29:565-70. [Crossref] [PubMed]
- Weitlauf AS, Sathe N, McPheeters ML, Warren ZE. Interventions Targeting Sensory Challenges in Autism Spectrum Disorder: A Systematic Review. Pediatrics 2017. [Crossref] [PubMed]
- Lanning BA, Baier ME, Ivey-Hatz J, et al. Effects of equine assisted activities on autism spectrum disorder. J Autism Dev Disord 2014;44:1897-907. [Crossref] [PubMed]
- Lofthouse N, Hendren R, Hurt E, et al. A Review of Complementary and Alternative Treatments for Autism Spectrum Disorders. Autism Res Treat 2012;2012:870391. [Crossref] [PubMed]
- Danial JT, Wood JJ. Cognitive behavioral therapy for children with autism: Review and considerations for future research. J Dev Behav Pediatr 2013;34:702-15. [Crossref] [PubMed]


