
Dyslexia: neurobiology, clinical features, evaluation and management
Neurobiology of reading
Neurobiology helps scientists to characterize different regions of the brain and study their respective functions. Taking a closer look at neural organization can help determine the internal processes that contribute to various neurological disorders. Neurobiology can be examined either through postmortem pathological studies or through in vivo neuroimaging studies. Neuroimaging can provide objective information which other tests cannot, in order to help understand how the brain works, or doesn’t work, with reading (1). Reading is a complex cognitive task that requires integration and communication across various regions of the brain (2) and generally happens with great automaticity despite the fact that the human brain is not generally hard-wired to do so (3).
The brain has two types of network organizations that are particularly implicated in reading: dense intra-connected modules, called resting state networks (RSNs), and hub areas that convey information between these RSNs (4). Areas of the brain required for reading are distributed across RSNs and an efficient architecture of RSN networks is required in order to carry out complex reading (4). The networks of the left hemisphere of the brain are crucial for reading, and there are certain regions of the brain that form significant aspects of these networks: the left inferior frontal region, the dorsal temporoparietal region, and the ventral occipitotemporal region (5). The dorsal attention network is where visual words are formed and the posterior temporal sulcus connects visual and auditory networks to associate letters with their respective sounds. Further, the inferior frontal gyrus has various subdivisions that aid in analyzing language syntax (4).
One model of reading posits that with initial single-word reading, a particular network begins to form wherein the superior temporal regions, important for processing phonetics, form connections with the temporoparietal regions of the brain, implicated in associating spelling and linguistic structures with the corresponding spoken language (5). The left ventral occipitotemporal circuit then becomes specialized for print and rapid word processing, which allows for sight word recognition, and a visual word form area (VWFA) then begins to develop, which is a critical region for visual processing. The VWFA demonstrates greater efficiency for processing of familiar words as inferred by higher levels of activation on functional MRI (fMRI) with visual input of familiar words (6). Thus, with extensive reading practice the ventral circuit becomes more automatic for reading. The anterior inferior frontal circuit also demonstrates increased development and utilization with age and reading practice. It is associated with various functions related to reading including phonological processing, comprehension, and speech planning. It is also important for general cognitive functions such as attention and inhibition (5).
Neurobiology of dyslexia
Dyslexia is an alternate term for a specific learning disorder with impairment in reading and is characterized by problems with accurate or fluent word recognition, poor decoding, and poor spelling abilities (7). A fundamental knowledge of the various brain regions that are implicated in reading disorders can guide administration of appropriate tailored interventions that may lead to an improvement in reading in those with dyslexia. The challenge in conclusively defining the neurobiology of dyslexia is borne from the construct that phonological deficit has multiple components (phonological awareness, impaired lexical retrieval and poor verbal short-term memory), each of which involves different neural networks (8).
Earlier studies documented differences between dyslexic and control brains, in the left perisylvian cortical and underlying white matter, thalamus, corpus callosum, and cerebellum (9). One theory was that the development of dyslexia is preceded by a failure of neuronal migration (10) from the ventricular zone up towards the cortical plate. While molecular genetic studies conducted in the early and mid-2000s on postmortem human brains supported this hypothesis, later studies were not able to produce the same results nor find a link between mouse models (10).
Currently, dyslexia is considered to be due to a defect in the ability to integrate information across different functional systems and is specifically associated with abnormal functioning of the hub region that connects information between different systems and RSNs (4). Several structural changes in the brain have been found that are associated with dyslexia. There is a global reduction in the neuroplasticity of the brain, particularly in the crucial left hemispheric regions that are implicated in language and reading (11). The right-sided counterparts of these brain regions are also often involved in structural brain changes. This results in specific cognitive impairments based on the regions that are affected, with a decreased openness to learning (11).
Increased myelination of the left perisylvian cortex is often seen with dyslexia (12). This region encompasses Broca’s area (associated with speech production) and Wernicke’s area (important for speech comprehension). Those at risk for dyslexia are shown to have reduced gray matter and cortical thickness, especially of the areas surrounding the perisylvian cortex at junctions of the parietal, temporal, and occipital lobes (13). Additionally, there is a hypoactivation of the left inferior frontal, temporoparietal, and occipitotemporal regions of the left hemisphere (5,13), the same areas that are responsible for recognizing symbols and letters, translating sounds into phonological meaning, and associating letters with sounds (4).
The brain changes are seen in children with dyslexia even when compared to children at similar reading levels without dyslexia. This indicates that people with this disorder have unique structural characteristics and are not simply characterized by delayed development of the brain (13). In children with a family history of dyslexia, various changes are seen early in development such as abnormal sulcal patterns and neural connectivity, including decreased white matter of the arcuate fasciculus (5,13). Certain regions of the brain also reach peak maturation earlier than normal in those with dyslexia, including the posterior corpus callosum and the temporoparietal region of the left hemisphere (which is part of the reading network) and right hemisphere (which makes up the attentional networks) (11). These two networks are connected because, during reading, the visual system must incorporate new information into existing language and comprehension networks. With increasingly complex text, the attentional circuits become increasingly engaged with the task and there is more global activation of centers throughout the brain (4). The corpus callosum is an inter-hemispheric structure that is critical in transmitting information from one hemisphere of the brain to the other. While consistent findings in the exact change in shape and size of the corpus callosum have not been established, dyslexia is associated with various morphological changes in the corpus callosum, which may help explain the deficiencies in complex processing that are characteristic of this disorder (2). While dyslexia has mostly been thought to be due to cortical alterations, recent studies have implicated subcortical structures including reduced corticothalamic connectivity in auditory (14) and visual systems (15).
The variation in research studies can be explained by the fact that persons can have phonological deficits in other disorders such as language disorders and attention-deficit hyperactive disorder (4,16,17). In children with dyslexia, there is a range of receptivity to begin learning to read and a large spectrum of resilience across individuals, which may account for the variation that is seen with these disorders (11).
Evidence-based phonics-based, and other structured reading interventions, have been found to be the most effective treatments in achieving either recovery (normalization of weak reading processes), compensation (alternative brain mechanisms that lead to an improvement in reading), or both (18). Not only have these interventions demonstrated an observable improvement in reading and language skills, but they lead to increased neural connectivity and activity, or hyperactivation, in the brains of people with dyslexia (18,19). In order to compensate, novel neural pathways may be recruited as well (18). These changes can be seen in previously hypoactive areas as demonstrated by fMRI (19). Further, auditory or phonological interventions have been shown to increase amplitude in oscillatory brain activity as measured by electroencephalogram (EEG), as well as alter brain structure by enhancing white matter integrity (19).
The areas that appear to be implicated by having a functional and structural improvement following interventions are the left thalamus, left middle occipital gyri, bilateral inferior frontal gyri, right insula, and right posterior cingulate gyrus (19,20). Interestingly, the content and type of intervention may make a difference in the brain area that is affected. In a study conducted by Heim et al., interventions that were focused on either phonology, attention, or reading (visual word recognition) all improved reading performance to a similar degree and increased activation of the VWFA (21). However, phonological and reading interventions increased activation in bilateral parietal areas, whereas attention training increased activation in the left temporal cortex (21). Thus, various reading training programs with different focuses can have both common and specific effects on brain activation, which is not necessarily evident by behavior alone.
The current body of literature endorses a plethora of brain regions that may be implicated in compensation and recovery, suggesting that there is either a large range of changes that can occur with reading interventions or that further research is still needed to establish the exact changes that take place with such interventions. As these research findings continue to be elucidated, they can help tailor and enhance existing interventions so that such treatment modalities may be able to maximally benefit individuals with dyslexia.
Clinical features of dyslexia
Dyslexia has an estimated prevalence ranging from 5% to 17% of school-aged children (20,22). The challenges in phonological processing, or recognizing single language sounds and single word decoding (23-25) cause these skills to come less naturally in children with dyslexia, and they subsequently develop challenges with reading, spelling, writing, and vocabulary acquisition (23,24,26). The degree of difficulty is variable; however, it is more than expected for an individual’s cognitive level and age, persists despite appropriate reading instruction, and has a chronic course (27).
Despite some of the neurobiological (and genetic) correlations, dyslexia is still a clinical diagnosis, with no definitive biochemical or neuroimaging markers, and there is no one test that can diagnose it (25,28). Diagnosis is based on history, observation, and psychological assessment. This diagnosis should be considered when there is a differential and unexpected lag between a person’s reading ability and their overall cognitive abilities, and there are associated challenges in phonological processing (23). Children with dyslexia can gain and acquire reading skills; however, reading is often more effortful (25), and their overall reading achievement is lower on average when compared with children without dyslexia (23,25). It is important to characterize children’s reading and diagnose dyslexia early, because early intervention with targeted reading remediation can improve reading outcomes (23,28). Additionally, as children and adolescents with dyslexia have increased risk for school failure, academic underachievement, and internalizing problems (anxiety, depression), appropriate interventions may prevent these secondary adverse events (25,28).
The typical progression for acquisition of reading skills is important to understand in order to serve as a comparison for the delays that may occur in individuals with dyslexia. In the toddler years, vocabulary and syntax development (forming sentences) often exist in the context of language exposure in the early environment and sensitive, responsive caregiving (29,30). Therefore, in the toddler years, there are typically few differences in vocabulary gains between children with dyslexia and those without dyslexia (26,31). However, this starts to change in the preschool years even before children develop reading skills (32,33). One of the first prospective studies of children with positive family history for dyslexia found that at 30 months, children who later developed dyslexia had no differences in vocabulary, compared with controls without dyslexia who were matched for age and socioeconomic status. Yet, starting around 36 and 42 months, children who later developed dyslexia had more challenges in vocabulary and syntax compared to these controls (31,32). These children at 5 years of age had more apparent problems with letter knowledge, phonological awareness, and expressive vocabulary than their counterparts without dyslexia (31). To summarize, subtle differences in vocabulary and syntax in children, even starting in the preschool years, especially accompanied by a family history of reading challenges, may be a risk factor for dyslexia and may precede reading difficulties and a diagnosis of dyslexia in school-age (26,31,32). Therefore, when evaluating preschoolers with language delays, clinicians should refer to speech-language pathology for evaluation and intervention, assist families in navigating request for school services, and obtain a family history for dyslexia or reading difficulties (23). Additionally, clinicians should provide families anticipatory guidance to monitor and report on these children having difficulties with reading at school-age (31,33).
In kindergarten, children may present with difficulties in learning letter names and letter sounds (phonemes) (23). Distinguishing between transient reading difficulties and dyslexia can be challenging, given the developmental progression of typical reading. Clinicians encountering kindergarteners with reading challenges may wish to connect families to reading interventions in their local schools. In first grade, children may present with difficulties reading sight words (even words such as “a” or “an” may be laborious and slow), making slow progress with reading, or illegible handwriting. Second grade marks a substantial shift in the academic and school curriculum, when children graduate from “learning to read” to “reading to learn” (26,28). Some elementary school-age children present with difficulties in school performance (may not be specific to reading), somatic complaints which may result in school avoidance, and low self-esteem and efficacy (23). Even after reading interventions and learning decoding skills, children may continue to be slower and more effortful readers. These challenges can also be accompanied by difficulties in writing and note-taking (dysgraphia) (23). Adolescents presenting in high school may have some degree of fluency but continue to suffer from phonological deficit that makes reading slower and they do not catch up with their typically reading peers (34).
A common misconception is that letter reversal is diagnostic for dyslexia—this may occur in typically-developing children, especially before 7 years age (35). Another myth is that children can “outgrow” dyslexia; however, while dyslexia does persist into adulthood, they may learn to be proficient in words that are important to their daily functional life (e.g., profession) (23). Yet another myth is that dyslexia occurs mainly in English language, however it can occur in other orthographies as well (36).
Evaluation
When there are concerns around academic and school achievement and/or reading, dyslexia should be considered in the differential diagnosis (23,28). Often, the pediatrician or primary care provider encounters this situation during surveillance in an anticipatory guidance visit, or at a visit requested by a caregiver to discuss the concern (often raised by the school). Obtaining a comprehensive history is the initial step in evaluation for dyslexia. This may include parent/caregiver checklist around developmental skills and behavioral presentation, as well as developmental and medical history, and educational history (which includes school achievement, reading progress, and ability to spell) (23,28). It is important to review reading milestones based on age to understand comparison with same-age peers. For instance, clinicians should ask families about their child’s letter recognition in kindergarten, sight word reading in first grade, and children’s ability to read short picture books for comprehension in second grade (23,28). Because dyslexia is a largely heritable condition, obtaining a family history of reading difficulties in family members is important; up to 65% of children with dyslexia also have a parent with dyslexia (37). Some direct observations of a child’s skills can be elicited in the clinical encounter, using paper and pencil to assess children’s writing and spelling abilities (asking them to write their own name or spell simple words), using a sample of reading material from a book and asking them to identify letters, make corresponding letter sounds, and read words (23,28).
Definitive diagnosis of dyslexia is often done by speech-language pathologists, psychologists, reading specialists, and educational specialists. Often educational and learning evaluations can be completed through the United States public school system, which guarantees a free and appropriate public education to all children with disabilities. The evaluation might include testing of language and reading abilities, cognitive or IQ testing, speech and language evaluation, and/or social-emotional evaluations. Eligibility for these services depends on several factors including: (I) the individual needs of the child, and (II) state/federal thresholds for determining eligibility. These school services are funded by the federal Individuals with Disabilities Education Act (IDEA), which was re-authorized in 2004 and amended as recently as 2015 (38). The educational eligibility for dyslexia usually falls under “specific learning disability”. Given the common deficits, especially those affecting phonological processing, that speech-language disorders appear to play in dyslexia (39), at times it is valuable to get a speech-language evaluation by a qualified professional.
Because dyslexia is an underlying deficit in phonological processing, neuropsychological testing should focus on assessment of phonological processing. See Table 1 for examples of assessments used for this purpose. Apart from phonological processing, word decoding, comprehension, and fluency all are assessed by these tools to varying degrees. These assessments can be helpful in primary school-age children, but adults and adolescents with dyslexia may do well on tests of reading and identification of sight words (23,28). One assessment that may be helpful for older readers might be the Nelson-Denny Reading Test, which is administered under both timed and untimed settings, so it provides added information on the automaticity of reading (42).
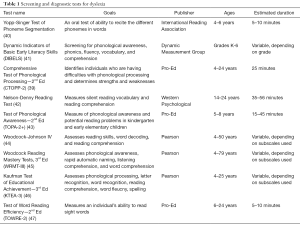
Full table
A medical evaluation should inquire into chronic medical conditions, which may be comorbid with dyslexia, and medications, which may impact alertness and hence learning. Some frequently co-occurring conditions include attention deficit hyperactivity disorder (ADHD) which can have a 20–40% co-occurrence, specific learning disability with impairment in mathematics (40% co-occurrence), and autism spectrum disorder (~30% co-occurrence) (43). It is key to conduct an audiologic evaluation and a vision evaluation to understand whether deficits in hearing or vision are compounding or causing the difficulties. Despite interesting neurobiological imaging findings, clinical brain imaging is not shown to be helpful in terms of diagnostic yield in dyslexia (36).
Management
Because dyslexia is a chronic condition, management often requires a life-span approach (28,48,49). There is no specific medication management or dietary supplementation for treatment of dyslexia (28,50). Optometric (e.g., vision therapy) and chiropractic interventions are not effective strategies for treating dyslexia (51). Treating underlying comorbid conditions is important, for example treatment of the ADHD can improve children’s school performance and ability to access the educational curriculum using medical and psychosocial treatments (52).
In the early academic years, management centers around remediation of the underlying reading problem (26,28,49,53). An initial step for children with more undefined reading challenges might include a response to intervention (RtI) reading trial, which involves additional reading practice outside of the classroom. If a child responds well to this intervention, then he/she may not require any additional instruction, and this may indicate that the child has a developmental lag in reading skills and not dyslexia. However, there are concerns about the RtI model in dyslexia, including the definition of “response”, the likelihood that bright, struggling readers may not be identified and that there is controversy about how best to implement a RtI framework (54). Also, it is important to note that RtI is not meant to delay adequate provision of services to children who need more support (55). More intensive intervention might include more reading instruction in a smaller classroom setting for a portion of the day, speech and language therapy, and/or supportive accommodations, which are discussed below. Often, children will require additional instruction outside of school due to the level of intensive intervention required for managing dyslexia. Such evidence-based interventions focus on building phonemic awareness (e.g., manipulating speech sounds into syllables and then words). Teaching should be explicit, completed by a tutor/reading specialist, preferably occurring in small groups with other children in similar skill levels (46,49). Lessons should systematically target instruction on only one or two phonemes at a time, build sequentially on skills, and include multisensory approaches (48,49). Examples of instructional programs include the Orton-Gillingham method, Barton reading program, and Wilson reading system. When delivered outside of educational systems, these types of programs are often not covered by medical insurance, are intensive, and require out-of-pocket payments. However, previous literature has shown that when applied, children’s reading skills improve significantly (48,49).
The next step following mastery of phonemic awareness is teaching phonics (e.g., letter to sound correspondence and spelling) (49,56). Once phonics are mastered, focus should be on reading (23,28), which is the ability to read with accuracy and speed (57,58) so that children become so accustomed to automatic word recognition that their cognitive resources are spent on understanding text passages (comprehension), as opposed to the act of reading itself (28,57,58). Prior literature has identified fluency as an important goal and teaching fluency includes routine practice with oral reading with immediate feedback from an instructor (28,57,58). Exposure to a wide range of vocabulary through audible books, storybook reading, and repeated exposure to words outside of school can help provide opportunities for lexical complexity and rich vocabulary (23,28). Though reading comprehension is also an important target goal to consider, evidence-based interventions for reading comprehension specifically are more limited (49).
In the later school years (secondary school and college), educational accommodations are the focus of management; however, it is never to late to attempt remediation strategies (28,59). Please see Table 2 for detailed descriptions around accommodations, different types of accommodations include: presentation, response, setting, and timing. Additional time for test-taking and reading is critical, so as to allow time for decoding of words which does not come as naturally to children and adolescents with dyslexia (23,60). Other accommodations may include: recording lectures, consideration of oral examinations in lieu of written examinations (and in general presenting instructions in an auditory format), speech to text software and spell check, use of note takers and tutors, and audiobooks (Learning Ally is one app-based audiobook library) (25,60).
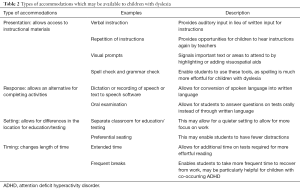
Full table
Modifications differ from accommodations in that the latter does not alter the expectation for the student, while the former lowers the target skill and allows the student to demonstrate what he/she is capable of. A decision on which approach to use depends on the student’s educational support team, based on data of the student’s performance, trajectory and what interventions have been previously attempted.
Psychoeducation
Clinicians can advocate for their patients and families and coach them through the process of obtaining an educational evaluation in their local school districts. Helping families understand the importance of a written request for their child to be evaluated for special education services and sharing with them templates to do so can be valuable. Families can also be directed to local parent-to-parent resources and regional advocacy partners. One helpful resource for families includes the book, “Overcoming Dyslexia” by Dr. Sally Shaywitz, a leader in the field of dyslexia research (61). Understood.org is also a nice resource for families that provides additional information on how to navigate the school system, which supports/accommodations to request, and basic information on dyslexia. Additionally, the Learning Disabilities Association for America has information on local resources such as tutors, reading specialists, programs, and support groups in the community.
Conclusions
Reading is a complex cognitive task that requires integration and communication across various regions of the brain, and neurobiological studies reveal that there are characteristic findings in dyslexia, which is characterized by problems with accurate or fluent word recognition, poor decoding, and poor spelling abilities which impairs reading ability. Additionally, reading interventions can cause changes in the structure and function of the brain, and further research is needed to help examine the impact of interventions to maximally benefit individuals with dyslexia. The clinical features of dyslexia vary depending on age of presentation, but generally involve a disconnect between an individual’s reading ability and their overall cognitive abilities, especially against a background of challenges in phonological processing period. Children and adolescents with dyslexia have increased risk for school failure, academic underachievement, and other psychiatric problems. Hence, timely and accurate diagnosis is important, and usually begins with screening and identification of children needing further evaluation. Ruling out and treating co-occurring conditions and referral to appropriate specialists is the key role of the healthcare provider. Interventions generally involve remediation in earlier school years and accommodations in adolescents. Families should engage the educational systems for appropriate interventions and healthcare providers can guide on community resources and assist in educational advocacy.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kearns DM, Hancock R, Hoeft F, et al. The neurobiology of dyslexia. Teach Except Child 2019;51:175-88. [Crossref]
- Wajuihian SO. Neurobiology of developmental dyslexia part 2: a review of magnetic resonance imaging (MRI) studies of the corpus callosum. Optom Vis Dev 2012;43:191-7.
- Dehaene S. Reading in the brain: the new science of how we read. New York: Penguin, 2009.
- Bailey SK, Aboud KS, Nguyen TQ, et al. Applying a network framework to the neurobiology of reading and dyslexia. J Neurodev Disord 2018;10:37. [Crossref] [PubMed]
- Ozernov-Palchik O, Yu X, Wang Y, et al. Lessons to be learned: how a comprehensive neurobiological framework of atypical reading development can inform educational practice. Curr Opin Behav Sci 2016;10:45-58. [Crossref] [PubMed]
- Seghier ML, Maurer U, Xue G. What makes written words so special to the brain? Front Hum Neurosci 2014;8:634. [Crossref] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5). Washington: American Psychiatric Pub, 2013.
- Turkeltaub PE, Gareau L, Flowers DL, et al. Development of neural mechanisms for reading. Nat Neurosci 2003;6:767-73. [Crossref] [PubMed]
- Eckert M. Neuroanatomical markers for dyslexia: a review of dyslexia structural imaging studies. Neuroscientist 2004;10:362-71. [Crossref] [PubMed]
- Guidi LG, Velayos-Baeza A, Martinez-Garay I, et al. The neuronal migration hypothesis of dyslexia: a critical evaluation 30 years on. Eur J Neurosci 2018;48:3212-33. [Crossref] [PubMed]
- Kershner JR. Neurobiological systems in dyslexia. Trends Neurosci Educ 2019;14:11-24. [Crossref] [PubMed]
- Skeide MA, Bazin PL, Trampel R, et al. Hypermyelination of the left auditory cortex in developmental dyslexia. Neurology 2018;90:e492-7. [Crossref] [PubMed]
- Norton ES, Beach SD, Gabrieli JDE. Neurobiology of dyslexia. Curr Opin Neurobiol 2015;30:73-8. [Crossref] [PubMed]
- Tschentscher N, Ruisinger A, Blank H, et al. Reduced structural connectivity between left auditory thalamus and the motion-sensitive planum temporale in developmental dyslexia. J Neurosci 2019;39:1720-32. [PubMed]
- Müller-Axt C, Anwander A, von Kriegstein K. Altered structural connectivity of the left visual thalamus in developmental dyslexia. Curr Biol 2017;27:3692-8.e4. [Crossref] [PubMed]
- Gori S, Molteni M, Facoetti A. Visual illusions: an interesting tool to investigate developmental dyslexia and autism spectrum disorder. Front Hum Neurosci 2016;10:175. [Crossref] [PubMed]
- Wallace MT, Stevenson RA. The construct of the multisensory temporal binding window and its dysregulation in developmental disabilities. Neuropsychologia 2014;64:105-23. [Crossref] [PubMed]
- Peck F, Leong A, Zekelman L, et al. Compensatory skills and dyslexia: what does the science say? 2018. Available online: https://dyslexiaida.org/compensatory-skills-and-dyslexia-what-does-the-science-say/
- Ylinen S, Kujala T. Neuroscience illuminating the influence of auditory or phonological intervention on language-related deficits. Front Psychol 2015;6:137. [Crossref] [PubMed]
- Peterson RL, Pennington BF. Developmental dyslexia. Lancet 2012;379:1997-2007. [Crossref] [PubMed]
- Heim S, Pape-Neumann J, van Ermingen-Marbach M, et al. Shared vs. specific brain activation changes in dyslexia after training of phonology, attention, or reading. Brain Struct Funct 2015;220:2191-207. [Crossref] [PubMed]
- Shaywitz SE, Shaywitz BA, Fletcher JM, et al. Prevalence of reading disability in boys and girls. Results of the Connecticut longitudinal study. JAMA 1990;264:998-1002. [Crossref] [PubMed]
- Shaywitz SE, Shaywitz BA. Dyslexia (specific reading disability). Pediatr Rev 2003;24:147-53. [Crossref] [PubMed]
- Thompson PA, Hulme C, Nash HM, et al. Developmental dyslexia: predicting individual risk. J Child Psychol Psychiatry 2015;56:976-87. [Crossref] [PubMed]
- Lyon GR, Shaywitz SE, Shaywitz BA. A definition of dyslexia. Ann Dyslexia 2003;53:1-14. [Crossref] [PubMed]
- Vellutino FR, Fletcher JM, Snowling MJ, et al. Specific reading disability (dyslexia): what have we learned in the past four decades? J Child Psychol Psychiatry 2004;45:2-40. [Crossref] [PubMed]
- Bruck M. Persistence of dyslexics’ phonological awareness deficits. Dev Psychol 1992;28:874. [Crossref]
- Shaywitz SE, Gruen JR, Shaywitz BA. Management of dyslexia, its rationale, and underlying neurobiology. Pediatr Clin North Am 2007;54:609-23. [Crossref] [PubMed]
- Hart B, Risley TR. Meaningful differences in the everyday experience of young American children. Baltimore: Paul H Brookes Publishing, 1995.
- Golinkoff RM, Hoff E, Rowe ML, et al. Language matters: denying the existence of the 30-million-word gap has serious consequences. Child Dev 2019;90:985-92. [Crossref] [PubMed]
- Scarborough HS. Early syntactic development of dyslexic children. Ann Dyslexia 1991;41:207-20. [Crossref] [PubMed]
- McCardle P, Scarborough HS, Catts HW. Predicting, explaining, and preventing children’s reading difficulties. Learn Disabil Res Pract 2001;16:230-9. [Crossref]
- Snowling M, Bishop DVM, Stothard SE. Is preschool language impairment a risk factor for dyslexia in adolescence? J Child Psychol Psychiatry 2000;41:587-600. [Crossref] [PubMed]
- Shaywitz SE, Fletcher JM, Holahan JM, et al. Persistence of dyslexia: the connecticut longitudinal study at adolescence. Pediatrics 1999;104:1351-9. [Crossref] [PubMed]
- Blackburne LK, Eddy MD, Kalra P, et al. Neural correlates of letter reversal in children and adults. PLoS One 2014;9:e98386. [Crossref] [PubMed]
- Ziegler JC, Perry C, Ma-Wyatt A, et al. Developmental dyslexia in different languages: Language-specific or universal? J Exp Child Psychol 2003;86:169-93. [Crossref] [PubMed]
- Scarborough HS. Predicting the future achievement of second graders with reading disabilities: contributions of phonemic awareness, verbal memory, rapid naming, and IQ. Ann Dyslexia 1998;48:115-36. [Crossref]
- Yell ML, Shriner JG, Katsiyannis A. Individuals with disabilities education improvement act of 2004 and IDEA regulations of 2006: implications for educators, administrators, and teacher trainers. Focus Except Child 2006;39:1-24.
- Pennington BF, Bishop DVM. Relations among speech, language, and reading disorders. Annu Rev Psychol 2009;60:283-306. [Crossref] [PubMed]
- Yopp HK. Yopp-Singer Test of Phoneme Segmentation. Read Teach 1995;49:20-9. [Crossref]
- Kaminski RA, Good RH III. Toward a technology for assessing basic early literacy skills. School Psych Rev 1996;25:215-27.
- Brown JI. The Nelson-Denny Reading Test. Oxford: Houghton Mifflin, 1960.
- Hendren RL, Haft SL, Black JM, et al. Recognizing psychiatric comorbidity with reading disorders. Front psychiatry 2018;9:101. [Crossref] [PubMed]
- Schrank FA, Mather N, McGrew KS. Woodcock-Johnson IV Tests of Achievement. Rolling Meadows: Riverside, 2014.
- Woodcock RW. Woodcock Reading Mastery Tests, Third Edition (WRMT-III). San Antonio: Pearson, 2011.
- Breaux KC, Lichtenberger EO. Essentials of KTEA-3 and WIAT-III assessment. Hoboken: John Wiley & Sons, 2016.
- Torgesen JK, Wagner RK, Rashotte CA. Test of Word Reading Efficiency—Second Edition (TOWRE-2). Austin: Pro-Ed, 2012.
- Torgesen JK, Wagner RK, Rashotte CA, et al. Preventing reading failure in young children with phonological processing disabilities: group and individual responses to instruction. J Educ Psychol 1999;91:579. [Crossref]
- Torgesen JK, Alexander AW, Wagner RK, et al. Intensive remedial instruction for children with severe reading disabilities: Immediate and long-term outcomes from two instructional approaches. J Learn Disabil 2001;34:33-58. [Crossref] [PubMed]
- Siegel LS. Perspectives on dyslexia. Paediatr Child Health 2006;11:581-7. [Crossref] [PubMed]
- American Academy of Pediatrics. Learning disabilities, dyslexia, and vision. Pediatrics 2009;124:837-44. [Crossref] [PubMed]
- Germanò E, Gagliano A, Curatolo P. Comorbidity of ADHD and dyslexia. Dev Neuropsychol 2010;35:475-93. [Crossref] [PubMed]
- Foorman BR, Breier JI, Fletcher JM. Interventions aimed at improving reading success: an evidence-based approach. Dev Neuropsychol. 2003;24:613-39. [Crossref] [PubMed]
- Reynolds CR, Shaywitz SE. Response to intervention: ready or not? Or, from wait-to-fail to watch-them-fail. Sch Psychol Q 2009;24:130. [Crossref] [PubMed]
- US Department of Education Office of Special Education Programs (OSEP). A response to intervention process cannot be used to delay-deny an evaluation for eligibility under the Individuals with Disabilities Education Act (IDEA). Available online: https://www2.ed.gov/policy/speced/guid/idea/memosdcltrs/osep11-07rtimemo.pdf
- Galuschka K, Ise E, Krick K, et al. Effectiveness of treatment approaches for children and adolescents with reading disabilities: a meta-analysis of randomized controlled trials. PLoS One 2014;9:e89900. [Crossref] [PubMed]
- Chard DJ, Vaughn S, Tyler BJ. A synthesis of research on effective interventions for building reading fluency with elementary students with learning disabilities. J Learn Disabil 2002;35:386-406. [Crossref] [PubMed]
- Wolf M, Katzir-Cohen T. Reading fluency and its intervention. Scientific Studies of Reading 2001;5:211-39. [Crossref]
- Tressoldi PE, Lorusso ML, Brenbati F, et al. Fluency remediation in dyslexic children: does age make a difference? Dyslexia 2008;14:142-52. [Crossref] [PubMed]
- Shaywitz SE. Dyslexia. N Engl J Med 1998;338:307-12. [Crossref] [PubMed]
- Shaywitz SE. Overcoming dyslexia: a new and complete science-based program for reading problems at any level. New York: Knopf, 2003.


